Steroid INJECTIONS
"A steroid injection is part of an overall treatment plan."
Inflamed painful joints may be treated with a corticosteroid injection. This reduces the inflammation associated with conditions such as osteoarthritis, tendonitis, bursitis, rheumatoid arthritis and gout. Corticosteroid injections, commonly called “cortisone,” have been used by doctors for over 60 years for a variety of conditions. Corticosteroid is naturally produced in the body through the adrenal gland and released when the body is under stress. A steroid injection will not necessarily treat the underlying condition. For example, osteoarthritis and rheumatoid arthritis may be treated with an injection but not cured.
A steroid injection is part of an overall treatment plan.
Injectable steroid is synthetically produced and is similar to the body’s own product. The benefits of the steroid injection to a joint typically lasts weeks to months but results vary widely. This temporary relief of pain may allow the patient to treat an arthritic flareup, participate in a physiotherapy supervised strengthening programme or postpone potential surgery. It is recommended to try and stay as close as you can to your ideal bodyweight to help weightbearing joints.
FAQs
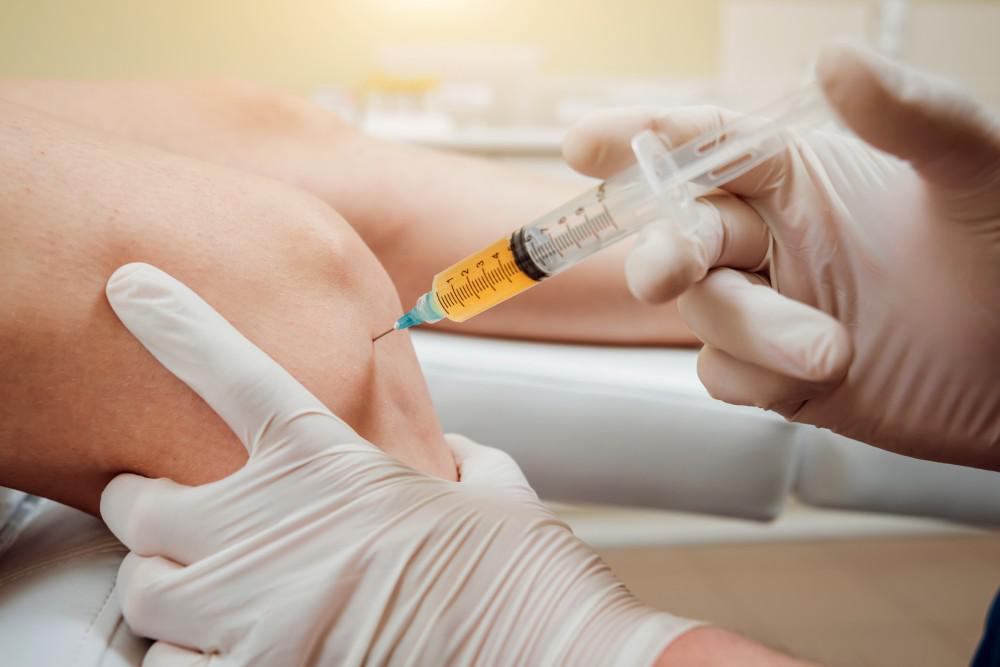
A steroid injection is not a pain-relieving medication, but rather works by minimising the body’s reaction to inflammation. When the inflammation is lessened, the pain is also reduced. By injecting the medicine directly into the inflamed area, such as a knee or shoulder joint, high concentrations of a steroid may be administered with minimal side effects. Discomfort usually improves within a few days and the injection lasts for several weeks, months or even permanently. If steroid injections are used, they must be combined with the appropriate rest period and rehabilitation to gain the best results. Activity after a steroid injection should be gradually increased.
There are very few contraindications in the use of steroid injections. However, the following conditions should be fully discussed with your doctor before seeking a steroid injection:
- Skin infection at the site of the injection
- Allergic reaction to previous steroid injections
- Usage of blood thinners, such as warfarin
- Acute injury (trauma, broken bones)
- Infection of a joint (septic arthritis)
Repeated steroid injections may affect soft tissues and joints. Most doctors prefer to wait at least 3 to 4 months before repeating any injection or considering surgery. Steroid injections become less effective in arthritic joints as the joint continues to wear with time rather than the joint becoming “immune” to steroid injections. Finally, athletes should not receive steroid injections into a joint or bursa sac immediately before competition, as the athletic activity may cause the injury to resurface, resulting in pain, swelling, and stiffness.
As with nearly any procedure where medications are injected into the body, adverse reactions may occur. The so- called “steroid flare” reaction has been reported to occur in approximately two percent of patients. This occurs when the injected steroid crystallizes and causes pain worse than before the shot. Fortunately, these “flares” usually do not last long and resolve with icing after 12 to 48 hours.
Whitening of the skin around the injection site can occur in <5% of people, may be permanent but is not harmful. Similarly, steroid can cause fat cells at the injection site to atrophy or waste away leading to a depression in the skin. It usually returns to normal after six months but can take 2 to 3 years. This side effect occurs in less than 1% of injections.
Additional side effects include softening of cartilage and weakening of tendons at the injection site. This usually occurs in patients who receive shots on a weekly-to-monthly basis, during a period of months to years. Most surgeons currently recommend having injections at least three months apart and avoiding repeat injections within a short-time period.
Diabetic patients may experience a temporary, but significant, elevation in blood sugar due to absorption of the steroid into the bloodstream. Diabetic patients should therefore carefully monitor blood sugar levels for 24 to 48 hours following an injection.
Although rare, infection at the injection site is another side effect. This may be avoided with through skin sterilisation.
